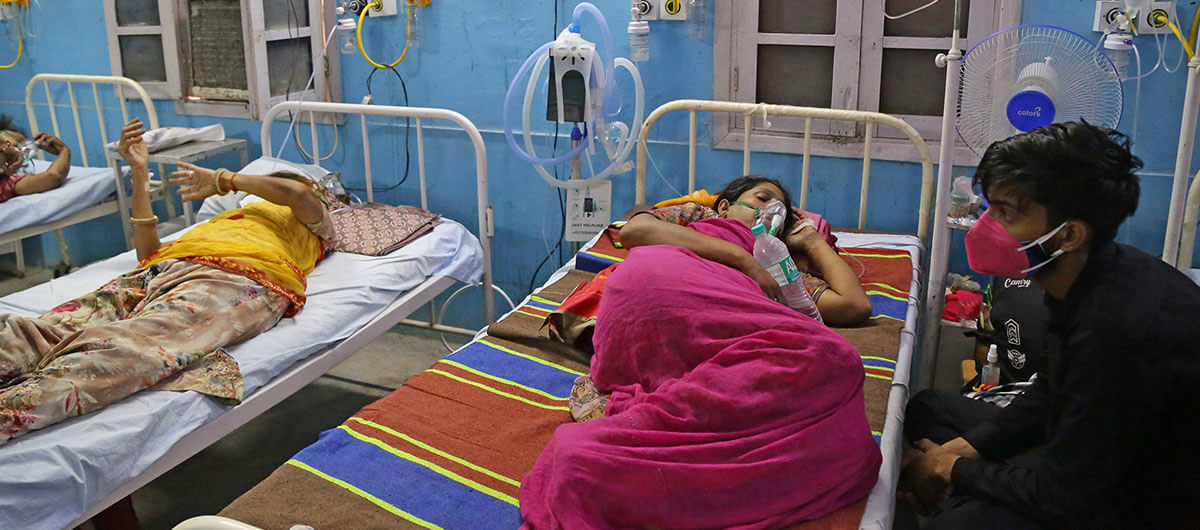

Sumit Saraswat/Shutterstock
International News
Sumit Saraswat/Shutterstock
India Is Battling More Than COVID
The pandemic’s toll on the country sparked another gruesome epidemic: black fungus—an infection whose treatment can be as brutal as the illness.
This article was made possible because of the generous support of DAME members. We urgently need your help to keep publishing. Please join us for as little as $1.00 a month or make a one-time gift in any amount!
In late March, Anjali Biswas, a 75-year-old resident of Pune, India, with a history of diabetes and heart problems, contracted COVID-19. By early April, as India was battling a brutal second wave of the pandemic, Biswas noticed her left eye had become swollen, and her vision was blurry. She’d been admitted to the hospital for COVID-19 treatment, but the overworked doctors hadn’t noticed her eye, so her granddaughter Sneha Gopalan had her moved to another hospital, where maxillofacial surgeon Dr. Pushkar Gadre was able to diagnose her: She’d developed a flesh-and-bone-eating fungus called “mucormycosis,” also known as “black fungus.” Unfortunately it was too late: Biswas had already lost her vision in that eye.
India is still in the grips of fighting the COVID pandemic, made more dangerous by dire shortages of hospital beds and critical medical supplies, the Modi government’s failure to prepare for the second wave, and, according to neurosurgeon Dr. Sachin Mahajan, what got them there in the first place: “The population’s ignorance to social distancing rules, callous attitude toward the disease and its transmission, virus mutations enabling them to transmit easily, social gatherings in large numbers have resulted in a large number of people getting infected.” But now India, which has a population of 1.4 billion people, has been hit with another epidemic as a result: black fungus, a secondary infection with a 50 percent mortality rate that is attacking people who have recently recovered from COVID.
“‘Black fungus’ is a misnomer,” explains maxillofacial surgeon Dr. Kiran Gadre, who works with his son, Dr. Pushkar Gadre, also a maxillofacial surgeon. The senior Dr. Gadre explains that the fungus is actually white, but the rare infection got its name because it is found in dead tissue “which makes it look black.” It invades the blood vessels, causing blood clots. Black fungus is caused by rhizopus and mucor species of fungi, which are commonly found all around us—in the soil, air, and decaying matter like compost. Which is to say, there is nothing unique about these spores—we breathe them every day. But if your immune system is compromised, these fungi can cause infection. And for those whose bodies have been weakened by COVID, it can be fatal.
According to Dr. Rajiv Sahay, a microbiologist and Director of Environmental Diagnostics Laboratory at Pure Air Control Services in Florida, the U.S. has seen some cases, but they’ve been so sporadic that “the CDC has yet to publish reports.” In recent months, Pakistan, Bangladesh, Russia, and Brazil, have reported a smattering of cases of black fungus, too, but nothing compared with what India is seeing—in just three weeks, they have seen numbers shoot up to 31,000 cases. ”Even before COVID-19, nearly 70 percent of global mucormycosis cases were reported from India,” says Dr. Akshay Nair, an oculoplastic surgeon. COVID simply compounded the nation’s health problems.
In his 40 years of practice, Dr. Kiran Gadre has treated about 70 patients infected by the deadly fungus—those patients were typically people who had untreated diabetes, or who were undergoing cancer treatment, or otherwise had compromised immune systems. During the first wave of the COVID pandemic, there were some cases trickling in of immunocompromised people developing black fungus. But the unprecedented rise in cases came during the second wave—the Health Ministry of India declared on May 20 that the black fungus is a “notifiable disease” under the Epidemic Diseases Act, 1897.
Experts can’t be entirely sure of what’s causing the uptick in cases. While Dr. Nair attributes the deadly black fungus to, among other things, the fact that “India has the largest number of undiagnosed diabetics, which could play a role in the infection,” recent reports suggest that sharp increase would appear to be due to an overburdened medical system, leading to a lack of hospital beds and a desperate shortage of medical oxygen. Some doctors, eager to save the lives of their patients, have been administering steroids for COVID patients who need oxygen because the steroids help reduce the inflammation in the lungs, helping patients breathe. But it’s not meant for longtime usage (more than ten days).
According to reports, the long-term usage of steroids is a double-edged sword, because while it provides COVID patients who can’t access medical oxygen with a way to breathe, it comes with the risk of weakening immune systems further, so that they’re not only susceptible to fungal spores, but also increasing blood sugar levels which renders diabetic people vulnerable. Worse yet, extended use of steroids could lead to blood clotting and therefore malnourished tissue, which fungus then attacks.
“COVID-19 itself is leading to an increase in diabetes among patients,” says Dr. Nair. He explains this isn’t always the case, but it can be a trigger. “Even if the blood sugar is well maintained, patients have acquired mucormycosis,” says Dr. Mahajan. Experts have questioned the administration of high doses of steroids for an extended period to COVID patients. “Understanding who needs steroids, giving the precise amount, and monitoring blood sugar is critical; otherwise, the patient [can be] susceptible to mucormycosis,” says Dr. Nair.
Black fungus isn’t typically contagious—the fungus is contracted by inhaling the mold spores. And early symptoms initially present like the common cold, namely nasal congestion and a runny nose. Then it affects the mouth: discoloration of the hard palate; swollen gums; abscessed teeth. Gums may discharge pus; teeth may even loosen. While the fungus often attacks the lungs, skin, and gastrointestinal tract, mucormycosis, like COVID, cleaves to the lining of the sinuses, which becomes their host tissue. Once the sinuses are infected, it spreads to the space around the eyes, erodes the bone, the surrounding mucosa, and blocks the blood vessels—and if it goes untreated for too long, it can spread to the brain. “It is highly invasive and reaches the brain through the skull base in a matter of a few days,” says Dr. Mahajan, who has been treating patients suffering from the black fungus. “Once it spreads to the brain, the survival rate drops from 80 percent to 50 percent,” adds Dr. Mahajan.
Once the infection spreads to the eyes, people may experience double vision, drooping eyelids, and loss of sight. If it travels to the brain, the patient experiences severe headaches, convulsions, paralysis of cranial nerves, unconsciousness, and an inability to respond to commands due to what’s called “altered sensorium,” a medical condition characterized by an inability to concentrate or think clearly.
And what’s worse is the excruciating treatment to stop further infection: First, doctors must perform surgery, a physically disfiguring process called debridement, to remove the dead tissue, says Dr. Girish Parmar, Director and Dean of Government Dental College and Hospital of Ahmedabad. An ear, nose, and throat surgeon does this endoscopically to remove all the infected tissue in the sinuses. Or, if it involves the eye, an oculoplastic surgeon or a maxillofacial surgeon will perform the operation. Along with the eye, they have to remove all the surrounding fungal tissue—the eyelid, the muscles, and fat around the eye. “If you leave behind any fungal infection, it has the potential to spread into the brain,” says Dr. Nair. “So, you have to be extremely aggressive. You leave behind a bony socket.”
A maxillofacial surgeon may also have to remove part or all of the upper jaw. In the case of Anjali Biswas, her infection had spread beyond her eye, so Dr. Pushkar Gadre and Dr. Murarji Ghadge, an ear, nose, and throat surgeon, had to remove her left upper jaw, and partial right upper jaw. Once all the infected tissue is taken out, the patients need a 15-day course of an injectable antifungal medication called amphotericin B in the immediate weeks following surgery.
Patients require hospitalization to administer amphotericin B injection, with dextrose and saline daily for 21 to 42 days. And they also need to monitor kidney function, blood pressure, and blood sugar levels during this course. But because of the surging cases of black fungus, India has an acute shortage of amphotericin B—each patient requires between 60 to 100 vials. Dr. Ghadge says that the dearth of medicines “is forcing patients to travel intercity and inter-state for treatment.” On June 29, it was reported that Gilead Sciences, the American company who manufactures the antifungal drug, is expected to supply 1 million doses to India.
If a patient has healed completely about three months after surgery and there appears to be no recurrence, then doctors can fit them with a cosmetic facial prosthetic. Still, patients do suffer trauma from the disfiguring, and often painful surgery, not to mention financial setbacks from the exorbitant cost of the treatments.
Dr. Sahay says immunocompromised COVID patients are also susceptible to other kinds of fungal infections, including white fungus, yellow fungus, and Aspergillosis. Nannizziopsis, found in reptiles like lizards, causes yellow fungus, which have emerged in India. White fungus, brought on by a yeast strain called Candida auris (C. auris), causes bloodstream infection and even death. The Pan American Health Organization issued an Epidemiological Alert due to the white fungus outbreak in the Americas in February. According to the CDC, since the start of the COVID-19 pandemic, outbreaks of C. auris have been reported in COVID-19 units of intensive care units. Inhaling Aspergillus fungal spores—mold found both indoors and outdoors—causes Aspergillosis infection, and compromises the lungs of COVID-19 patients.
Dr. Sahay explains that these thrive in hot and humid conditions. “Monitoring humidity and temperature in the air-conditioning system helps inhibit mold growth indoors. Periodic maintenance of the heating, ventilation and air conditioning system also helps in ensuring the fungus does not proliferate.” Avoiding damp areas, wearing clean masks, maintaining oral hygiene, getting regular blood sugar tests done are a few steps that could help reduce the probability of fungal infections in COVID-19 patients.
Today, Anjali Biswas is thankfully on a slow road to recovery. Not everyone has gotten there. After the unrelenting devastation the people of India have faced with the deadly pandemic, and the growing epidemic of mucormycosis and other fungal infections, the nation’s recovery is hard to see right now. We can only hope this will sound the alarm to prepare, with the necessary medical supplies, well enough to prevent a third wave before it threatens to descend upon us.
Before you go, we hope you’ll consider supporting DAME’s journalism.
Today, just tiny number of corporations and billionaire owners are in control the news we watch and read. That influence shapes our culture and our understanding of the world. But at DAME, we serve as a counterbalance by doing things differently. We’re reader funded, which means our only agenda is to serve our readers. No ads, no both sides, no false equivalencies, no billionaire interests. Just our mission to publish the information and reporting that help you navigate the most complex issues we face.
But to keep publishing, stay independent and paywall-free for all, we urgently need more support. During our Spring Membership drive, we hope you’ll join the community helping to build a more equitable media landscape with a monthly membership for as little as just $1.00 per month or a one-time gift in any amount.

























































































